Effective Hair Transplantation Solutions Available in the UK
For individuals residing in the United Kingdom, there are effective and safe methods to achieve the desired hair restoration without the need to travel to Turkey. Various primary techniques exist that offer natural-looking results, enabling individuals to regain their confidence. This information seeks to provide insights into these methods and their benefits.
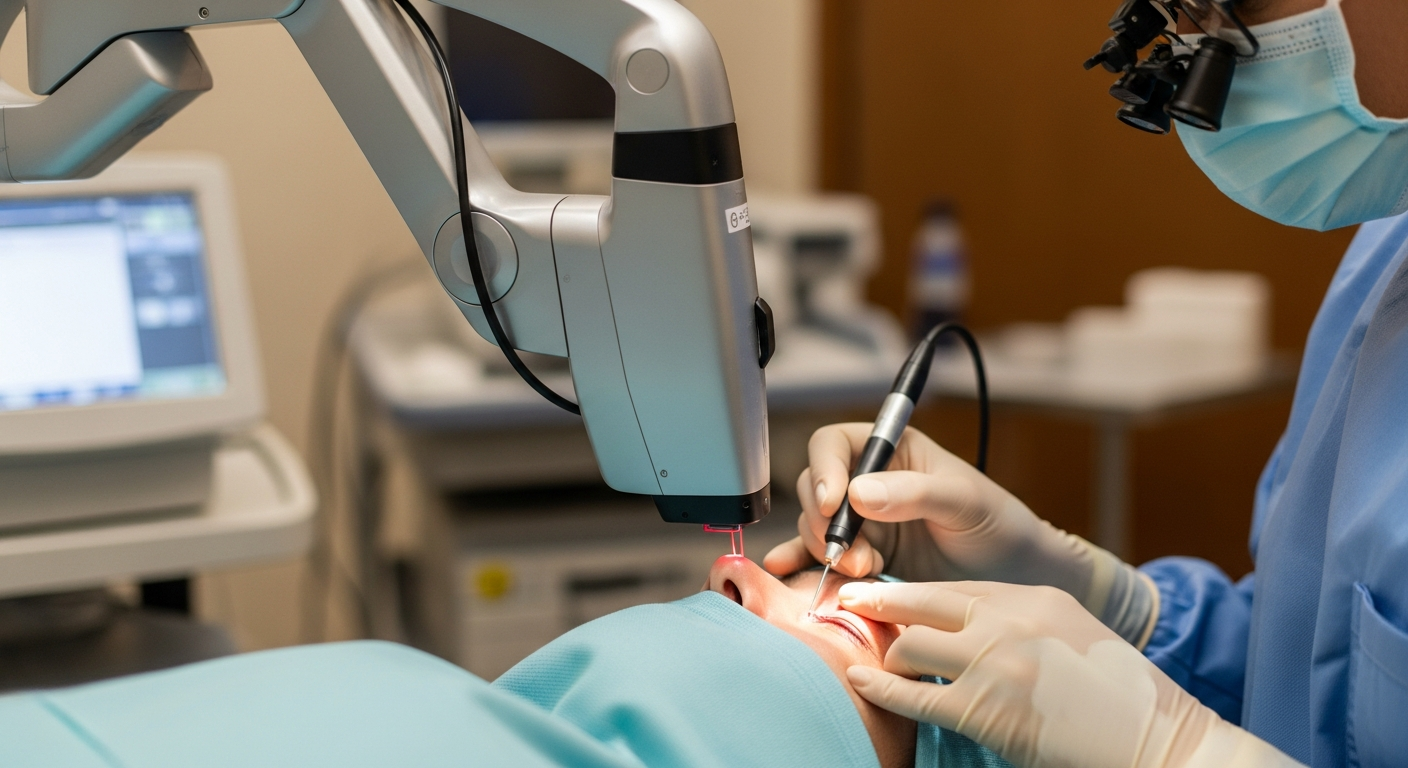
For many people in the United Kingdom, progressive thinning can affect confidence, styling choices, and day-to-day routines. Modern surgical restoration aims to redistribute resistant follicles to areas of loss, but results depend on careful planning, technique, and realistic expectations about density and timelines.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How UK transplantation techniques work in practice
In UK clinics, the two most established surgical approaches are FUE (Follicular Unit Extraction) and FUT (Follicular Unit Transplantation, often called strip surgery). Both relocate follicular units from a donor area (usually the back and sides of the scalp) to recipient areas where thinning is visible. The key difference is how grafts are harvested, which influences scarring patterns, session length, and suitability for different hairstyles.
FUE removes individual follicular units using small punches, leaving many tiny dot scars that are often less noticeable with shorter hair. It can be well suited to people who prefer closely cropped styles or those who want to avoid a linear scar. FUT removes a thin strip of scalp from the donor area, and the follicles are dissected under magnification; it leaves a linear scar that may be concealed with longer hair and can be an option when a larger number of grafts is needed in a single session.
In either method, natural-looking design depends on the plan for the frontal hairline, the angle and direction of placement, and how grafts are distributed to match existing density. UK consultations commonly include an assessment of donor capacity, current loss pattern, family history, and the likelihood of future thinning, since surgery typically needs to “work with” progression rather than assume it stops.
Benefits of choosing local hair restoration over overseas options
One reason some patients prefer local hair restoration over overseas options is continuity of care. Hair transplantation is not only a day-of-surgery decision; it involves pre-operative assessment, clear consent, and post-operative follow-up to monitor healing and early growth. Being treated in your area can make it easier to attend review appointments, address unexpected swelling or irritation, and discuss shedding or growth concerns without travel pressure.
Regulation and accountability are also practical considerations. In the UK, surgical practice is shaped by professional standards, and clinics are typically expected to provide transparent information about who performs each part of the procedure, including harvesting and implantation. Patients can ask direct questions about the clinician’s role, experience with similar cases, and how complications are managed. This clarity can matter because outcomes can be affected by team skill, graft handling time, and the consistency of technique.
Local care can also reduce logistical strain. Long-haul travel soon after surgery may be uncomfortable, and crowded environments increase the chance of knocking or contaminating the recipient area. While many overseas clinics provide competent care, comparing like-for-like is difficult if consultation time is brief, communication is rushed, or follow-up is limited once you return home.
Achieving natural-looking results with advanced methods
Natural-looking outcomes are usually the product of planning rather than any single “advanced” tool. Surgeons often use magnification to protect graft integrity and to place follicular units in a pattern that mimics how hair naturally groups (single hairs at the very front, then gradually more multi-hair units behind). The hairline is typically designed to suit face shape and age, with irregular micro-variations rather than a straight, dense border.
Density expectations are important. A transplant redistributes finite donor hair; it does not create new follicles. Many plans therefore prioritise the frontal frame first, then mid-scalp, and finally crown work if donor supply permits. The crown can require substantial grafts for modest visual change because of its swirl pattern and the way light hits the scalp.
Aftercare influences how well grafts survive the first critical days. Typical advice includes gentle washing routines, avoiding friction, and limiting heavy exercise for a period advised by the clinic. Shedding of transplanted hairs in the first weeks can be normal, with visible regrowth often taking months; clinics frequently describe the early period as a healing and stabilisation phase rather than an immediate transformation.
Medication can also be part of a long-term strategy, particularly when ongoing thinning is likely. Some patients discuss evidence-based medical options with a qualified clinician to help maintain non-transplanted hair, because a strong transplant result can look uneven if surrounding hair continues to miniaturise.
What a UK consultation and screening should include
A thorough UK consultation usually covers medical history, scalp health, and whether hair loss is stable enough for surgery. Certain conditions (for example, inflammatory scalp disorders) may need treatment first. The clinician should explain risks such as infection, prolonged redness, numbness, shock loss (temporary shedding of nearby hairs), and scarring, as well as what can and cannot be corrected in a revision.
Planning should also include a donor assessment. Donor density, hair calibre, curl pattern, and colour contrast with the scalp affect the final appearance. People with very limited donor supply may be advised to consider non-surgical cosmetic options or a more conservative surgical plan to avoid overharvesting.
It is also reasonable to ask how the clinic documents results. Consistent photography, similar lighting, and clear timelines help set expectations. Be cautious with comparisons that do not show the same angles, hair length, or time since surgery.
Recovery, timelines, and realistic expectations
Recovery varies, but most people have visible signs of the procedure in the first days, such as redness and small scabs in the recipient area. Many can return to desk-based work relatively quickly, while roles involving helmets, dust, or heavy physical activity may require longer adjustments. The donor area can feel tight or sore, and sleeping positions may be modified for comfort.
The growth timeline is often slower than expected. It is common for transplanted hairs to shed after implantation, with new growth emerging later. Final appearance typically evolves over many months as thickness increases and hairs mature. Because future thinning may continue, long-term planning matters as much as early results; a conservative hairline and sensible density distribution can age more naturally.
In the UK context, the most “effective” solution is usually the one that fits your pattern of loss, donor supply, health status, and capacity for follow-up. A credible plan should balance aesthetics with preservation of donor hair and a realistic view of maintenance over time.




